UnitedHealthcare & Walmart OTC | Healthy Benefits Plus
Login | Register | Enrollment
Company: United Healthcare (UHC) & Walmart
Support and resources for United Healthcare | Healthy Benefits Plus | Over The Counter | www.healthybenefitsplus.com/hwp:
Customer Service Support Phone Number is:
1-833-845-8798, TTY 711
Company Summary:
This company has partnered with Walmart to allow Eligible Members to make better use of their Over-The-Counter Benefit. Eligible Members of UnitedHealthcare will save on many over-the-counter (OTC) health items! The sponsored program they have created is called: Healthy Benefits Plus.
Healthy Benefits Overview:
This number is for questions and assistance regarding Healthy Benefits Plus. However, if you have questions about your health insurance plan or coverage, please call the number found on your current health plan ID card. You must be an eligible United Healthcare member to register for Healthy Benefits Plus.
Use the programs website to access your OTC benefits anywhere, anytime.
Online Access
You can instantly redeem your benefits on qualifying products with your card number or barcode when ready to checkout. To view your benefit information and get details on how to shop, see below.
It is a very easy online process.
You can also find your program website information in the welcome materials that were sent to you in the mail. Be sure to review your welcome materials. Also login to your program website for a full description of benefits and shopping options.
By submitting this form, you are consenting to receive marketing emails from: HealthManagementCorp (HMC). You can revoke your consent to receive emails at any time by using the Unsubscribe link, found at the bottom of every email. By using this form, you acknowledge that you have read and agree to the Privacy Policy and Terms & Conditions.
What is the United Healthcare Over-The-Counter Benefit?
It is a preset money amount or allowance provided at no additional costs. It is for eligible members to use to purchase over the counter products. No money out of pocket is required. Again, there is an automatic allowance provided to spend on thousands of lower-priced OTC items. Items such as allergy medication, cough drops, first aid supplies, oral care, pain relievers, vitamins and much more!
Why use the UHC OTC Benefit?
You may choose from three different ways to shop:
Why create a Healthy Benefits Plus online account?
With the Healthy Benefits Plus online account you will be able to:
- View your allowance balance / amount left to use for the OTC benefit.
- Browse all items that are eligible.
- Use your UHC OTC card number or barcode to redeem benefits.
- Review the transaction history.
- Update your personal account information.
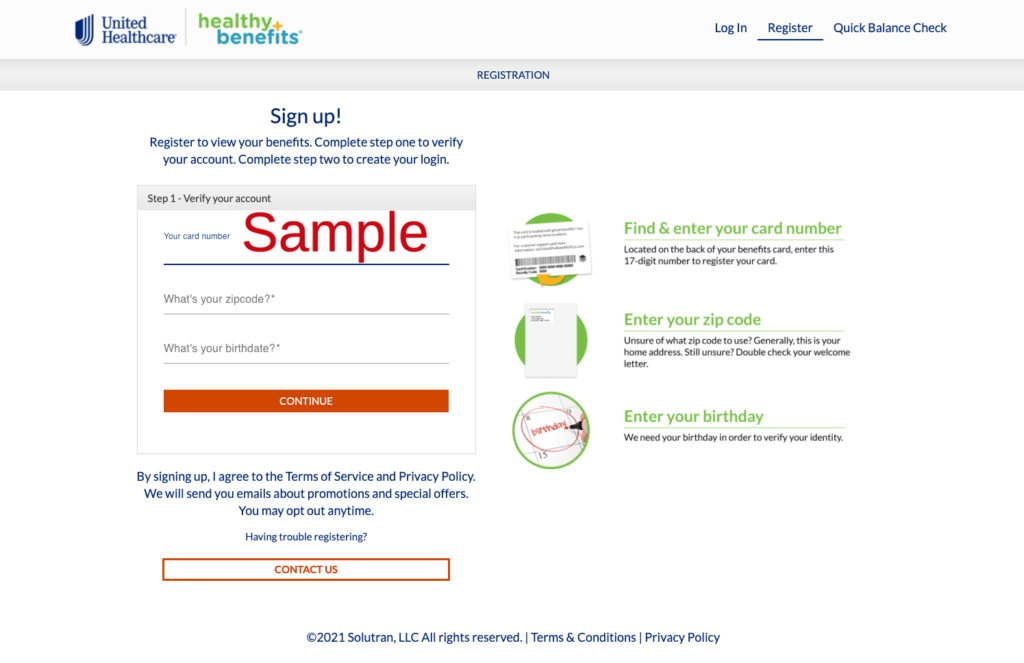
Create a New United Healthcare OTC Healthy Benefits Plus online account:
- Visit: https://www.healthybenefitsplus.com/hwp or click here.
- Click on the “Register” link located in the upper right hand area of the page.
- Type in and provide the following:
- 17 Digit card number.
- Your Zip Code.
- Your Date of Birth.
- Click on the “Continue” button.
- Continue to move forward and provide all the required information to verify your identity and complete the registration for a new online account.
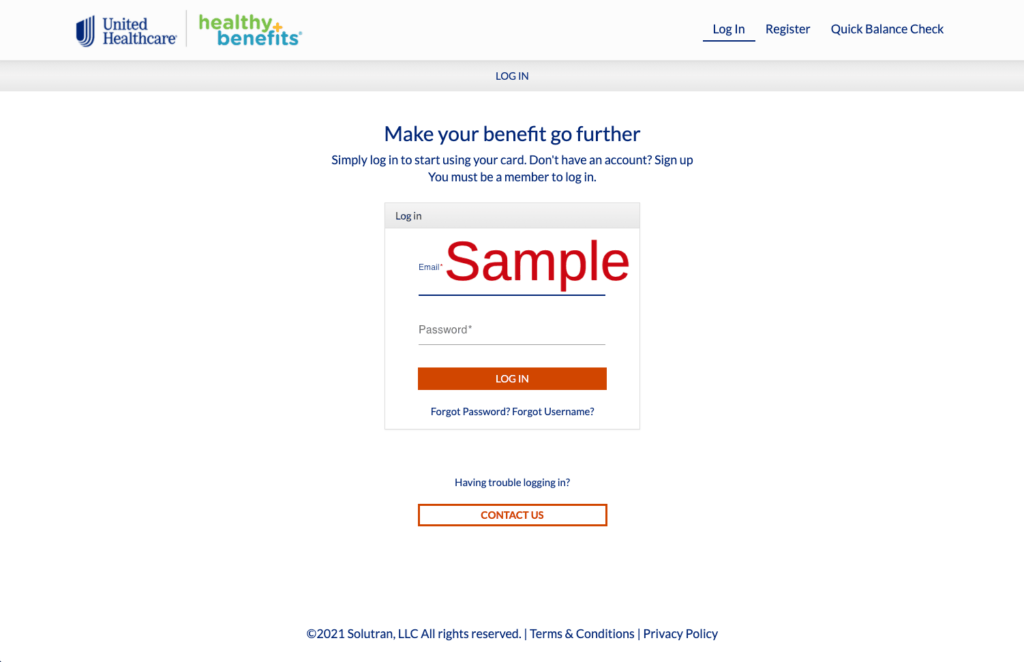
Login to a New United Healthcare OTC Healthy Benefits Plus online account:
- Visit: https://healthybenefitsplus.com/hwp.
- Click on the “Log In” button on the upper right hand area of the page.
- Type in the following in the fields provided:
- Your Email address.
- Your current password.
- Click on the orange “Log In” button and begin managing your current online account.
What to do AFTER you login or register online:
-
First
- To create an order online first explore the thousands of approved over-the-counter health products. You can browse on the website, mobile app, or the OTC catalog. When you are ready to buy, simple click “Buy Online”.
-
Second
- You will then be transferred to Walmart.com to build a basket and complete your purchase. Also, you can create a Walmart.com account or checkout as a guest.
-
Third
- When you are at the checkout page, select the”Gift Card” option for payment.
-
Lastly
- Provide your 17-digit account number and 4-digit security code from the back of your OTC card.
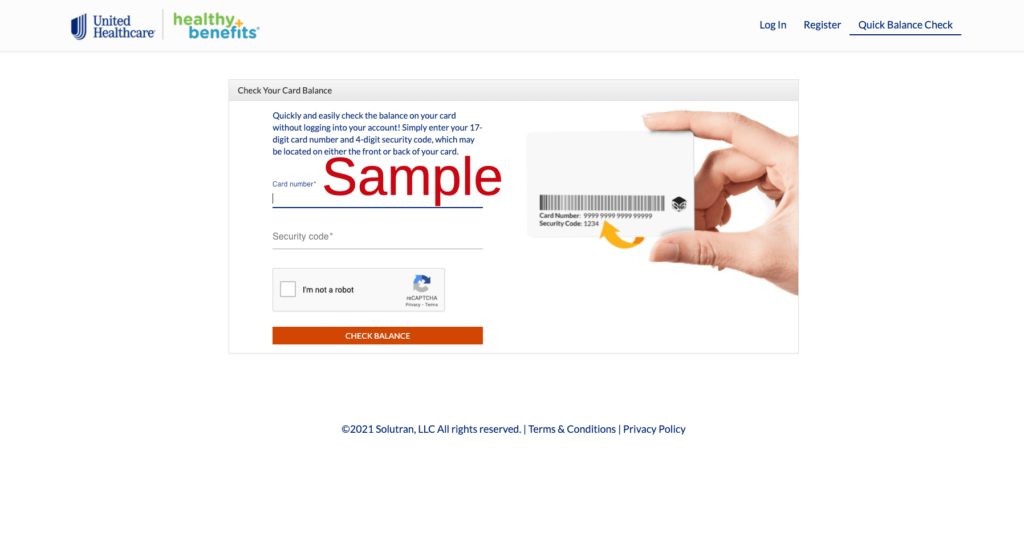
Use the Quick Balance Check Tool for your OTC Card:
- Visit: https://healthybenefitsplus.com/hwp/Account/BalanceCheck
-
Type in the following:
- your 17-digit card number
- your 4-digit security code
- Click on the “I’m not a robot” box.
- Click on the green “Check Balance” button.
Download the Healthy Benefits Plus App:
NOTE:
You should be able to download a copy of the catalog online or through the app.
United Healthcare Video Guide
Support and resources for United Healthcare | Healthy Benefits Plus | Over The Counter | www.healthybenefitsplus.com/hwp:
Customer Service Support Phone Number is:
1-833-845-8798, TTY 711
Company Summary:
This company has partnered with Walmart to allow Eligible Members to make better use of their Over-The-Counter Benefit. Eligible Members of UnitedHealthcare will save on many over-the-counter (OTC) health items! The sponsored program they have created is called: Healthy Benefits Plus.
Healthy Benefits Overview:
This number is for questions and assistance regarding Healthy Benefits Plus. However, if you have questions about your health insurance plan or coverage, please call the number found on your current health plan ID card. You must be an eligible United Healthcare member to register for Healthy Benefits Plus.
Use the programs website to access your OTC benefits anywhere, anytime.
Online Access
You can instantly redeem your benefits on qualifying products with your card number or barcode when ready to checkout. To view your benefit information and get details on how to shop, see below.
It is a very easy online process.
You can also find your program website information in the welcome materials that were sent to you in the mail. Be sure to review your welcome materials. Also login to your program website for a full description of benefits and shopping options.
Need Medicare or Health Insurance?
By submitting this form, you are consenting to receive marketing emails from: HealthManagementCorp (HMC). You can revoke your consent to receive emails at any time by using the Unsubscribe link, found at the bottom of every email. By using this form, you acknowledge that you have read and agree to the Privacy Policy and Terms & Conditions.
What is the United Healthcare Over-The-Counter Benefit?
It is a preset money amount or allowance provided at no additional costs. It is for eligible members to use to purchase over the counter products. No money out of pocket is required. Again, there is an automatic allowance provided to spend on thousands of lower-priced OTC items. Items such as allergy medication, cough drops, first aid supplies, oral care, pain relievers, vitamins and much more!
Why use the UHC OTC Benefit?
You may choose from three different ways to shop:
Why create a Healthy Benefits Plus online account?
With the Healthy Benefits Plus online account you will be able to:
- View your allowance balance / amount left to use for the OTC benefit.
- Browse all items that are eligible.
- Use your UHC OTC card number or barcode to redeem benefits.
- Review the transaction history.
- Update your personal account information.
Create a New United Healthcare OTC Healthy Benefits Plus online account:
- Visit: https://www.healthybenefitsplus.com/hwp or click here.
- Click on the “Register” link located in the upper right hand area of the page.
- Type in and provide the following:
- 17 Digit card number.
- Your Zip Code.
- Your Date of Birth.
- Click on the “Continue” button.
- Continue to move forward and provide all the required information to verify your identity and complete the registration for a new online account.
Login to a New United Healthcare OTC Healthy Benefits Plus online account:
- Visit: https://healthybenefitsplus.com/hwp.
- Click on the “Log In” button on the upper right hand area of the page.
- Type in the following in the fields provided:
- Your Email address.
- Your current password.
- Click on the orange “Log In” button and begin managing your current online account.
Need Medicare or Health Insurance?
By submitting this form, you are consenting to receive marketing emails from: HealthManagementCorp (HMC). You can revoke your consent to receive emails at any time by using the Unsubscribe link, found at the bottom of every email. By using this form, you acknowledge that you have read and agree to the Privacy Policy and Terms & Conditions.
What to do AFTER you login or register online:
-
First
- To create an order online first explore the thousands of approved over-the-counter health products. You can browse on the website, mobile app, or the OTC catalog. When you are ready to buy, simple click “Buy Online”.
-
Second
- You will then be transferred to Walmart.com to build a basket and complete your purchase. Also, you can create a Walmart.com account or checkout as a guest.
-
Third
- When you are at the checkout page, select the”Gift Card” option for payment.
-
Lastly
- Provide your 17-digit account number and 4-digit security code from the back of your OTC card.
Use the Quick Balance Check Tool for your OTC Card:
- Visit: https://healthybenefitsplus.com/hwp/Account/BalanceCheck
-
Type in the following:
- your 17-digit card number
- your 4-digit security code
- Click on the “I’m not a robot” box.
- Click on the green “Check Balance” button.
Download the Healthy Benefits Plus App:
NOTE:
You should be able to download a copy of the catalog online or through the app.